Charles Bonnet syndrome stroke

What is it?
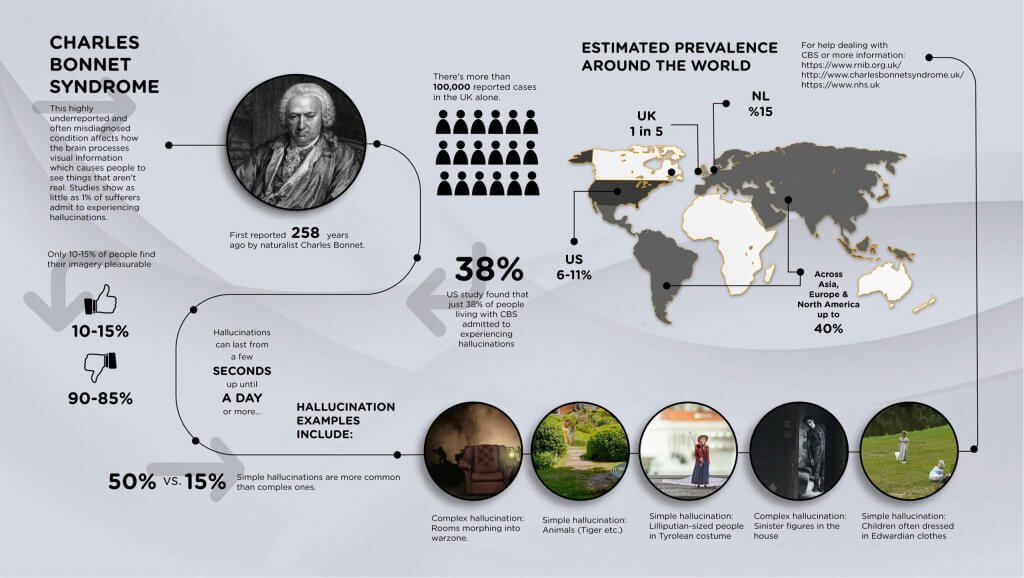
Charles Bonnet syndrome (CBS) is characterized by visual hallucinations in the absence of psychiatric pathology.
Advances in medicine and improved living standards have reduced the mortality rate, but the longer average life span, and therefore the aging of the population, predisposes the body to more pathologies, including visual pathologies.
The increase in the number of visually impaired patients in industrialized countries is mainly caused by optic-retinal diseases.
Charles Bonnet syndrome, first described in the 18th century, affects 60 percent of individuals with age-related macular degeneration. The macula, at an anatomical level, is the central area of the retina, responsible for the distinct vision of shapes and details; it contains the largest number of cones.
Pathogenetic theories
Several theories have been proposed that appear to play a role in the pathogenesis of Charles Bonnet syndrome:
- sensory deprivation: phantom vision
- perceptual release theory
- neuro matrix theory
- release hallucinations
- social isolation
- senescence
- psychological factors
- cerebral perfusion theory
A bit of history
The simplest manifestation is photopsia of various colors, but there are also the more complex hallucinations described by Charles Bonnet in the 1700s.
The Swiss scientist Charles Bonnet first described the syndrome in 1760, when he first discovered this phenomenon of visual hallucination in his 90-year-old grandfather.
The grandfather, after a cataract operation, appreciated an improvement in his vision; later, after his visit deteriorated, he noticed visual hallucinations.
The hallucinations were unreal and the grandfather did not suffer from psychiatric disorders.
Features
Charles Bonnet syndrome is a medical condition in which complex visual hallucinations occur in conjunction with visual changes, particularly loss of visual acuity while maintaining intact intellectual functioning.
As vision decreases, messages transmitted from the retina to the visual cortex slow down or stop altogether; the brain behaves oppositely, activating to create non-existent mental representations (visual hallucinations).
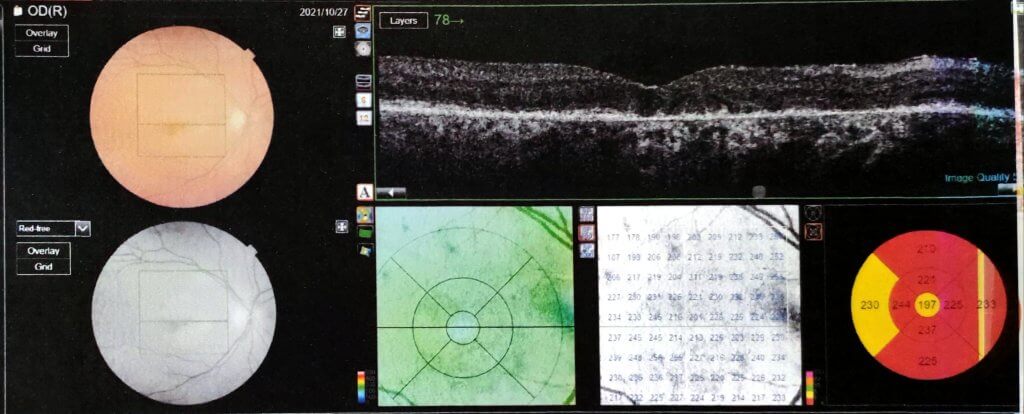
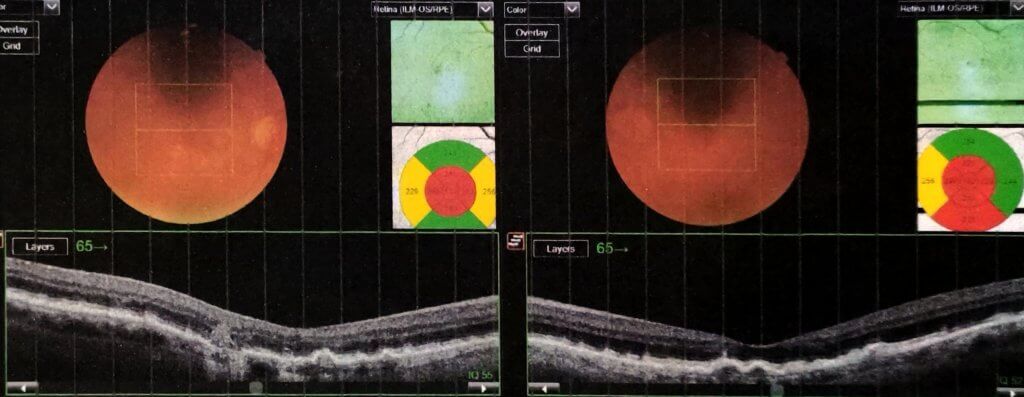
Charles Bonnet’s syndrome involves a release phenomenon caused by the suppression of afferent nerve impulses (deafferentation) to the visual associative areas of the cerebral cortex, resulting in phantom vision.
The brain misinterprets visual information, generating visions that can be debilitating and disturbing.
Simple manifestations include the vision of photopsia, also known as ‘phosphenes’ or bright visual sensations similar to flashes of light.
Structured manifestations include the vision of unfamiliar faces, flowers, and objects.
Hallucinations, whether structured or not, can also appear in individuals who have had retinal laser treatment.
Due to the nature of hallucinations and the most common aetiologies, Charles Bonnet syndrome often goes unrecognized and is misdiagnosed as early dementia or psychosis.
Patients are usually very reluctant to talk about their problems because they are concerned about a possible interpretation of a psychiatric disorder.
The patient is usually unaware of the unreality of the visual experiences; they may cause distress, but they are typically normal. Unfortunately, the patient has little or no control over hallucinations.
A detailed anamnesis is essential to exclude other pathologies.
Hallucinations may improve spontaneously or as vision improves.
Therapy
There is no drug of choice for Charles Bonnet syndrome. No drug is effective, however, anticonvulsants have been shown to improve or stop hallucinations.
The main task of the examiner is to comfort the patient about the unreal vision.
The awareness of the ophthalmologist and the patient are the key components of management.
Bibliography
- “Hallucinations Experienced by Visually Impaired: Charles Bonnet Syndrome”, L. Pang, 2016
- “Charles Bonnet Syndrome”, L. C. Rojas & B. Gurnani, 2022
- “Charles Bonnet Syndrome”, E. Nieman, 2018
- “Charles Bonnet Syndrome and Other Hallucinatory Phenomena”, F. Boller & D. S. Birnbaum et all, 2018
- “Charles Bonnet syndrome: a review”, A. P. Schadlu & R. Schadlu et all, 2009

You are free to reproduce this article but you must cite: emianopsia.com, title and link.
You may not use the material for commercial purposes or modify the article to create derivative works.
Read the full Creative Commons license terms at this page.