Visual impairment: how to recognize and identify it?

Trauma and injury can compromise visual information by generating visual impairment.
The central visual field deficits (also known as CVFD) are nothing more than alterations of our visual field. In these cases, it is of fundamental importance to be able to obtain a correct diagnosis so that we can understand and frame all the difficulties that each patient encounters.
Having in mind the visual deficits and the problems connected with them is fundamental when planning a rehabilitative or compensatory approach 1.
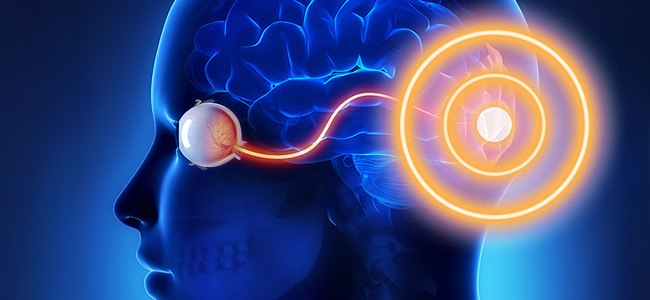
Oftentimes the functional part of the impaired visual field corresponds to an injured anatomical part: different types of functional alterations can give valuable information on the anatomical part of our compromised optical pathways, thus helping the doctor in the neuro-visual rehabilitation phase.
Le zone anatomiche prese in considerazione quando parliamo di DCCV sono quelle che partono dal chiasma ottico alla corteccia visiva primaria (nello specifico: chiasma ottico, tratto ottico, nucleo genicolato laterale, radiazione ottica e corteccia visiva primaria).
The anatomical areas taken into consideration when we talk about CVFD are those starting from the optical chiasm to the primary visual cortex (specifically: optical chiasm, optical tract, lateral geniculate nucleus, optical radiation and primary visual cortex).
What are the kinds of visual impairments?
- General field of view deficit: it can refer both to the loss of the central visual field (lesions or alterations from the optic chiasm onwards) and the loss of the peripheral visual field (retinal alterations to the optic nerve and the optical papilla).
- Scotoma: well localized and defined deficit of a portion of the visual field; it may present as a relative or absolute scotoma. Interestingly enough, all of us have a physiological scotoma (blind area) that corresponds to the retinal area where we have our optical papilla.
How to find our blind spot
Let’s carry out this simple and quick test to identify the blind spot that each of us has physiologically. Let’s start by covering one of the two eyes, for example, the left; now concentrate on observing the image shown in figure 1 (blind-spot image); make sure you are at about 30 cm from the screen and start fixing the cross with your eye. It is of fundamental importance not to make movements with the eyes.

At this point you begin to slowly approach the screen; the dot, located to the right of the image begins to disappear and reappear depending on your movements. The explanation of this kind of optical illusion is given by the image processing mechanism that takes place in the visual cortex: when the dot enters the blind spot of the right eye, our brain takes advantage of the surrounding area (which in the case of the image we are referring to is white) to compensate for the missing visual information. This simple test can be done with both eyes.
If you want to delve deeper into the topic of blind spot, we recommend watching Sara Cosenza‘s video.
We have addressed many concepts regarding the study of the visual field, both in functional and anatomical terms; although these basic aspects are very easy to understand and test (see blind spot test) there is still a lot to do and discover about the various types of visual deficits.
An issue of great complexity
This complexity is due to the fact that people with visual impairment have very different needs, which depend on a variety of factors such as:
- age
- the possible presence of residual visual capacity
- personal and social conditions
- The presence of other conditions associated with visual impairment.
Another complication that is generally associated with those who incur in this type of problem is a series of repercussions on their psychological and social well-being. Therefore, we try to intervene by trying to develop the other abilities of the person, making him in this way more self-sufficient and thus compensating for all those limitations that threaten to affect the autonomy of the individual.
We can ideally subdivide two classes
- blind;
- low vision: those who have reduced but present visual abilities; there are various situations that can lead to low vision and all of these differ according to the triggering pathology and its level of severity.
There is a further difference between those who are blind or visually impaired from birth and those who have acquired this condition with the passage of time. The absence of sight is in fact to affect a transient delay (then disappear in adolescence) in the development of certain functions, such as orientation in space.
Altro elemento da considerare risiede nell’analisi della condizione del paziente: se manifesta esclusivamente un deficit visivo puro oppure se quest’ultimo rappresenta soltanto una delle varie problematiche della persona. Distinzione fondamentale perché permette di delineare il quadro del paziente, fornendo utili indicazioni sul modo in cui il soggetto può attuare una compensazione mediante le altre sue facoltà sensoriali
Fortunately, day after day the scientific community acquires more and more information in the field of neuro-vision and neurovisual rehabilitation; this is already helping and will further aid present and future generations to live not only a long-lasting life but also a quality one.
Bibliography
- Deficit centrali di campo visivo | Ottobre 2015 | Roberto Facchin, Roberta Daini
- Ibid.

You are free to reproduce this article but you must cite: emianopsia.com, title and link.
You may not use the material for commercial purposes or modify the article to create derivative works.
Read the full Creative Commons license terms at this page.