Neglect: what is it, how to recognize it and how to cure it

The editorial staff of Emianopsia has the pleasure of hosting Dr Chiara Spatafora: graduated in Orthoptics and Ophthalmological Assistance with additional qualification in optics. Dr Spatafora offers us an insight about neglect.
Before starting you can listen to the speech Neglect: what is it, causes and rehabilitation principles by Dr. Casati, speaker of the webinar organized by Linari Medical.
What is the neglect?
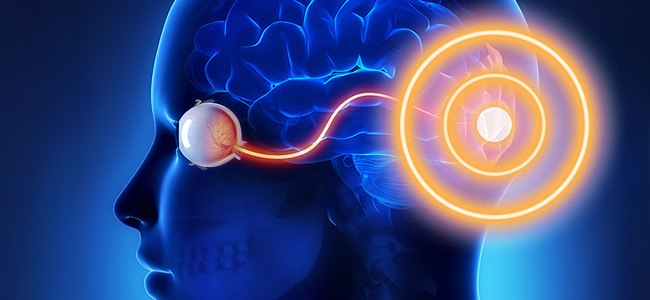
Unilateral spatial negligence is a neurocognitive disorder that can be defined as the inability to interact and respond to stimuli from a specific part of view field. It is a complex pathology that also embraces the psychological sphere, as it affects not only the perception that the patient has of the surrounding space, but sometimes also of his own body.
What is the root cause?
This deficiency occurs mainly because of stroke or brain trauma, causing the person to completely loses awareness of the contralateral space in the affected cerebral hemisphere.
In Italy, the general prevalence of stroke is 6.5%, and it is the third leading cause of death after cancer and heart disease. Nonetheless, we ought to remember that as many as 70% of patients who survive, a year after the stroke, maintain disabilities.
Stroke determines many deficits of a different nature: motor, visual and even psychiatric. Within the large group of visual alterations we find:
- hemianopsia (the loss of half the visual field);
- alteration of eye movements;
- neglect.
Location of the brain injury
Generally this pathology is associated with an injury of the right hemisphere so the patient will no longer have awareness of stimuli coming from the left, and in the contralateral space to the injury. The main cause is perfusion damage, such as ischemia and stroke.
This is a selective disorder because the person, unknowingly, ignores half of the space ( almost always that of the left side ). On the other hand, spatial negligence is rarely associated to an injury in the left hemisphere (which covers other fundamental functions related to the understanding and articulation of, thanks to the areas of Broca and Wernicke, and therefore not connected to space recognition).
It is recognized, statistically, that this deficit is manifested much more often, and in a much more serious form following injuries of the right hemisphere: between 33-85% is manifested following a stroke in the right hemisphere, whilst about 0-25% among stroke patients show neglect in the left hemisphere.
Neglect: spontaneous regression and chronic illness
This visual deficit is manifested in the acute phase of stroke so it can regress spontaneously, but in some cases unfortunately tends to become chronic. In a study conducted at the University of Bologna on a group of 23 patients, 43% of cases had a regression of the disorder in the post-acute phase of stroke, but only 9% had a total recovery (A. Farnè &co, 2004).
It is extremely complex to understand whether the disorder can regress by itself or become chronic, considering how many parameters must be taken into account:
- the location of the injury;
- its extent;
- severity of symptoms.
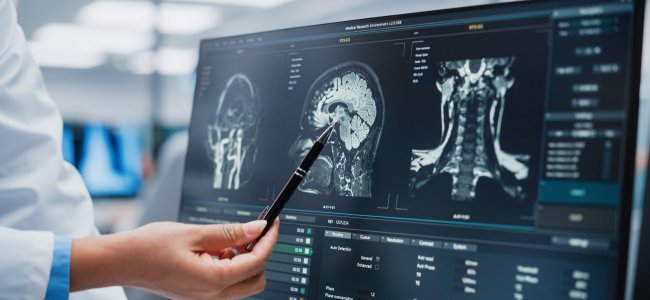
In the acute phase, while using neuro-diagnostic tests, it is almost impossible to pinpoint the exact location of brain damage because there might still be oedemas that have not been reabsorbed.
How to distinguish this pathology from other similar deficits?
In case of neglect, the patient does not perceive the objects present in the area opposite the injury, so he has a disorder that is part of the visual sphere, but it is essential to remember that there are lesions involving the optical pathways. Precisely for this reason it is necessary to make a differential diagnosis between neglect and hemianopsia: in the second case we have a loss of the visual field related to an anatomical injury in the optical pathways.
Precisely the most common form of post-stroke hemianopsia is the homonymous hemianopsia (for further information, please refer to the article “Lateral homonymous hemianopsia: the challenge posed to doctors”) that manifests itself due to a retro-chiasmatic lesion. Another fundamental difference is that patients with hemianopsia are aware of the loss of the visual field, while the one with spatial negligence usually have no awareness of their own deficit, defined as anosognosia. Anosognosia indicates a neuropsychological disorder in which the affected person does not realize they have a neurological disorder.
The patient with spatial negligence, in the diagnostic phase, could underestimate their difficulties in recognizing objects present in their left view field because they have no awareness of said deficit nor can they understand its importance. A peculiar characteristic of this pathology is the behaviour of the patient who moves their gaze and head spontaneously towards the space corresponding to the injury.
Within the group of neuromotor disorders that may resemble spatial negligence, we find the optical ataxia, which consists in the inability of the individual to interact with an object, creating a discrepancy between visual and motor coordination. The fundamental difference between the two conditions is that in optical ataxia, the patient remains aware of the presence of this object even if they cannot see or touch it.
The main kinds of spatial negligence
In relation to space, this pathology can be distinguished in:
- personal: in this case the patient no longer recognizes the left part of their own body: they may forget to wear makeup or shave the left side of the face, or to dress that part as well.
- peripersonal: peripersonal space indicates what is close but distinguished from their body; the patient with a lack of peripersonal space will find themselves leaving food on the plate on their left side.
- extrapersonal: in this case it represents the space that is farthest away from us and is alien to our body, for example, left visual field when driving.
How do we reach a diagnosis?
For the diagnosis, in addition to the CT scan to identify areas affected by stroke, one of the most used tests is the BIT test (Behavioural Inattention test).
These are test batteries ( both conventional and behavioural tests ) in which the patient is invited to perform exercises as similar as possible to daily actions: drawing geometrical figures, writing a phone number, or drawing a picture. Typically, in affected subjects, drawings represent only half of the object.
Unilateral spatial negligence: which are the treatments?
Over the years, different therapies have been studied and tested, not only for the complexity of the disorder, but also for the difficulty in verifying the effectiveness of the same therapy. Assessing the reliability of therapy is not taken for granted precisely because this visual deficit can resolve spontaneously.
Among the therapeutic approaches undertaken we find very different rehabilitative techniques:
- use of an occlusor;
- music therapy;
- prismatic adaptation;
- use of noradrenergic agonist drugs.
The prismatic adaptation
Prismatic adaptation is one of the most promising techniques, usually managed by a multidisciplinary team consisting of:
- neurologists;
- ophthalmologists;
- orthoptists.
Thanks to the use of left-based binocular prisms, which move the image of the observed objects to the right, and a rigorous rehabilitation process, we have been able to achieve a certain degree of improvement, which can last for weeks and sometimes months.
Bibliography
- What is a stroke – NIH review.
- Stroke Prevention and Educational Awareness Diffusion. Ictus cerebrale: linee guida di prevenzione e trattamento |SPREAD.
- Neglect and related disorders | Heilman.
- The assessment of visuo-spatial neglect after acute stroke | Stone.
- Visual impairment following stroke: do stroke patients require vision assessment? | Rowe.
- Patterns of spontaneous recovery of neglect and associated disorders in acute right brain-damaged patients| Farné et all.
- The anatomy of spatial neglect | Karnath.
- Visuo-spatio neglect: a systematic review of current interventions and their effectiveness | Laute.
- L’adattamento prismatico nella riabilitazione della negligenza spaziale unilaterale: una rassegna critica |A. Facchin.

You are free to reproduce this article but you must cite: emianopsia.com, title and link.
You may not use the material for commercial purposes or modify the article to create derivative works.
Read the full Creative Commons license terms at this page.